There were 102,371 respondents to the Smoking Toolkit survey from June 2017 to August 2022. He excluded 411 people (0.4%) who did not report smoking status, leaving him with a sample of 101,960 people for analysis. Of these, 55,349 were surveyed before the start of the pandemic (June 2017 to February 2020) and 46,611 were surveyed during the pandemic (April 2020 to August 2022). The proportion of cases missing for smoking cessation outcomes was small (4.1% for quit attempts and 0% for quit attempts, number of quit attempts, and use of support). Table 1 presents weighted descriptive statistics for the entire sample and as a function of pandemic timing (unweighted characteristics are shown in Additional file 5: Table S1).
current smoking
Table 2 summarizes the GAM results. Figure 1 shows current smoking trends during the study period.
Current smoking status (overall, by age, by social class). The panel shows trends in current smoking prevalence. a British adults (Unweighted n: Overall=101,960, ABC1=64,088, C2DE=37,872), B 18-24 years old (Unweighted n: Overall=12,455, ABC1=7766, C2DE=4689), and C 45-65 years old (Unweighted n: Overall=34,332、ABC1=22,401, C2DE=11,931), from June 2017 to August 2022. The line represents the modeled weighted prevalence over the study period, adjusting for covariates. Points represent unadjusted weighted prevalence by month. The vertical dashed line indicates the start of the coronavirus pandemic in the UK (March 2020). ABC1, Managerial/Professional/Intermediate. C2DE, small employer/lower supervisor/technical worker/semi-daily/daily/not working at all/long-term unemployed
Overall, among UK adults, the onset of the coronavirus disease (COVID-19) pandemic was associated with a negligible stage-level change in current smoking (Figure 1A). However, there was a notable change in trends.Before the pandemic, smoking prevalence was decreasing by 5.2% per year (relative risk, trend[RRtrend]= 0.948; Note that this percentage represents a relative percentage point decrease, not an absolute percentage point decrease. That is a decrease of 5.2% compared to the previous year. [(1-RR)*100], rather than a 5.2 percentage point decline within a given year). After the onset of the pandemic, this rate of decline slowed to 0.3% per year (RRtendency×RRΔtrend= 0.948 × 1.052 = 0.997; Figure 1A). The change in trends from pre- to post-pandemic was significant (relative risk, change in trends)[RRΔtrend]= 1.052, 95% confidence interval[CI]= 1.014, 1.090). The smoking rate in June 2017 was estimated at 16.2%. At the start of the pandemic (March 2020) it was 15.1%. In August 2022, it was almost flat at 15.0%.
Stratified analysis showed a gradual increase in smoking prevalence among socially advantaged adults (ABC1) by 20.1% (95% CI = 10.1, 31.0%) at the start of the pandemic, followed by a slowing of the pre-pandemic decline to the point where progress in smoking reduction shown to be reversed (+3.6% per year compared to -9.5% pre-pandemic, RRΔtrend= 1.145, 95% CI = 1.083, 1.211; Figure 1A). In contrast, among socially disadvantaged classes (C2DE) there was no increase in smoking prevalence, and the pre-pandemic slow (approximately 3% per year) decline appeared to continue (Figure 1A) .
When we looked at current smoking across different age groups, we found a variety of changes related to the pandemic. There was a stepwise increase of 34.9% (95% CI = 17.7,54.7%) for those aged 18–24 years (Figure 1B). However, there was a 13.6% (95% CI = 4.4, 21.9%) step-level decrease between ages 45 and 65 (Figure 1C). The increase in smoking prevalence among young adults was similar across social classes, but the decline in smoking prevalence among middle-aged adults was limited to those in socially disadvantaged classes (-22.4%, 95% CI = -10.7, -32.6%). As we observed overall, progress in smoking reduction stopped among more advantaged social strata during the pandemic (from -12.4% to -0.3% per year for 18-24 year olds, RR)Δtrend= 1.138, 95% CI = 1.004, 1.290; for ages 45 to 65, RR is – 11.7% to + 3.4% per yearΔtrend= 1.171, 95% CI = 1.055–1.300), but similar to pre-pandemic prevalence within disadvantaged social classes (Figures 1B and C).
The data showed that these changes persisted over time (Figure 1) rather than short-term pulse effects during the early months of the pandemic (Additional file 5: Table S3).
stop activities
Data on smoking cessation were available for all 17,964 people in the sample who smoked in the past year. There were 741 people (4.1%) with missing data regarding the number of termination attempts, and 0 of the subjects had missing data regarding the number of termination attempts. Table 2 summarizes the GAM results. Figure 2 shows trends in smoking cessation activities over the study period.
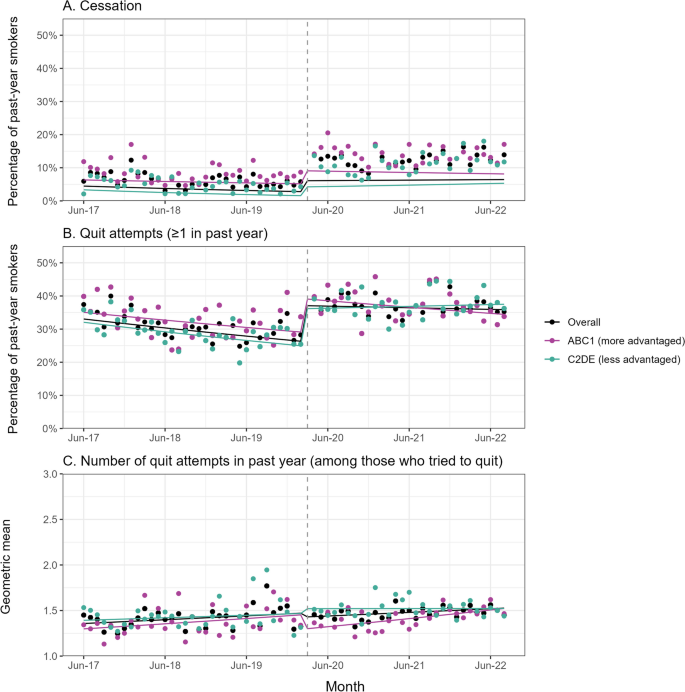
Cessation of activity overall and by social class. The panel shows trends in the prevalence of infectious diseases. a) canceled and B Among those who smoked in the past year, attempted to quit at least once in the past year (Unweighted n: Overall=17,964、ABC1=8802, C2DE=9162), and C Weighted geometric mean number of past year quit attempts among past year smokers who made at least one quit attempt (Unweighted n: Overall=5754, ABC1=2908, C2DE=2846), from June 2017 to August 2022. The line represents the modeled weighted prevalence (or mean) over the study period, adjusting for covariates. Points represent the unadjusted weighted prevalence (or average) by month. The vertical dashed line indicates the start of the coronavirus pandemic in the UK (March 2020). The corresponding data without adjusting for dependencies are shown in Additional file 5: Figure 1 and Additional file 5: Table 4. ABC1, Managerial/Professional/Intermediate. C2DE, small employer/lower supervisor/technical worker/semi-daily/daily/not working at all/long-term unemployed
Among past-year smokers, the pandemic was associated with a 120.4% (95% CI = 79.4-170.9%) increase in quit stage level (Figure 2A). This increase was despite the fact that when tobacco dependence was not adjusted (Additional file 5: Table S4, Additional file 5: Figure S1A), mean tobacco dependence decreased only slightly over the period by 154.4 % (95% CI = 104.8 to 216.1%). pandemic (Additional file 5: Table S5, Additional file 5: Figure S3). There were also changes in trends. Before the pandemic, the prevalence of smoking cessation was decreasing at a rate of 16.1% per year (RRtendency= 0.839); this rate of decline slowed during the pandemic (RRΔtrend= 1.219, 95% CI = 1.079–1.379) to 2.3% (Figure 2A). This change in trend was driven by socially disadvantaged groups, among whom quitting rates reversed from -24.5% per year before the pandemic to +9.8% per year during the pandemic (RR)Δtrend= 1.454, 95% CI = 1.200–1.762; Figure 2A). In contrast, the pre-pandemic, more modest (7.4%) decline in smoking cessation among people of social class appeared to continue (Figure 2A). This pattern of results was largely replicated when data from smokers aged 25 years and older were analyzed separately (Additional file 5: Table S6, Additional file 5: Figure S4). However, in a much smaller group of 18- to 24-year-olds, a significant increase in quit stage level was observed, although confidence intervals exceeded zero and point estimates from the overall analysis There was uncertainty in all of the results. Pre-pandemic outage trends, trend changes, and patterning of socio-economic outcomes (Additional file 5: Table S6, Additional file 5: Figure S4).
The pandemic was also associated with a step-level increase of 41.7% (95% CI = 29.7 to 54.7%) in the proportion of smokers in the past year who attempted to quit at least once (Figure 2B). This increase occurred at all ages, but was greater among smokers aged 18 to 24 (90.8%) [95% CI = 57.0–131.9%]) than people aged 25 and over (31.5%) [95% CI = 19.1–45.2%]) (Additional file 5: Table S6, Additional file 5: Figure S4). The rate of decline in quit attempts slowed from 8.2% to 1.4% per year (RRΔtrend= 1.074, 95% CI = 1.016–1.136; Figure 2B); again, this is driven by people in less advantaged social classes, with no significant change in trends among more advantaged social classes. (Fig. 2B) and was only observed among people aged 25 years and older (Additional file 5: Table S6; Additional file 5: Figure S4). Among those who attempted to quit, there was little change in the average number of attempts (Figure 2C).
Pulse effect analysis showed an increase in cessation activity in the first 2–3 months of the pandemic (Additional file 5: Table S3), as evidenced by visual inspection of the data in Figure 2 and changes in trend results (Table S3). 2) These increases persisted until August 2022.
Use of smoking cessation support
Table 2 summarizes the GAM results. Figure 3 shows trends in the use of smoking cessation support over the study period.
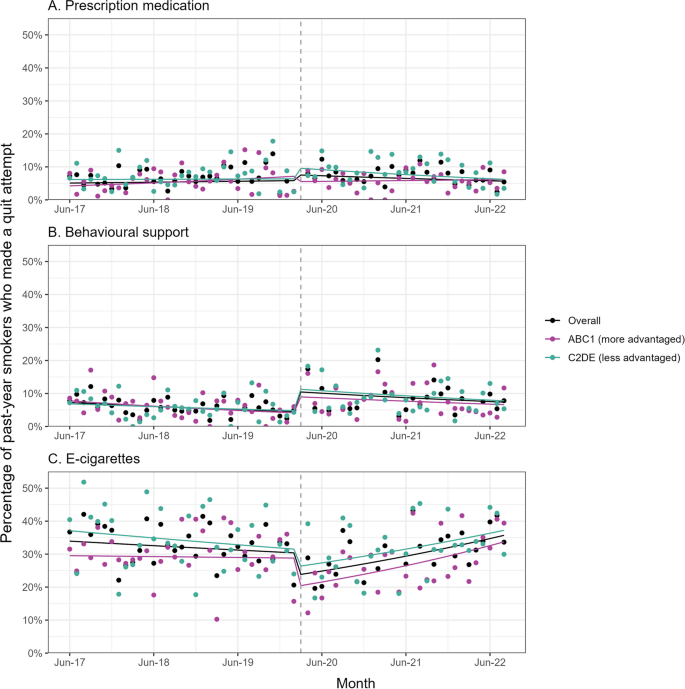
Smokers’ use of support when trying to quit, overall and by social stage. The panel displays trends in the prevalence of usage. a Prescription drugs, B behavioral support, and C Among smokers who have attempted to quit smoking at least once in the past year, recent attempts to quit using e-cigarettes (Unweighted n: Overall=5754, ABC1=2908, C2DE=2846), from June 2017 to August 2022. The line represents the modeled weighted prevalence over the study period, adjusting for covariates. Points represent unadjusted weighted prevalence by month. The vertical dashed line indicates the start of the coronavirus pandemic in the UK (March 2020). The corresponding data without adjusting for dependencies are shown in Additional file 5: Figure 2 and Additional file 5: Table 4. ABC1, Managerial/Professional/Intermediate. C2DE, small employer/lower supervisor/technical worker/semi-daily/daily/not working at all/long-term unemployed
Among smokers who attempted to quit in the past year, there was little change in the onset of the COVID-19 pandemic and prescription drug use (Figure 3A). Score estimates for step-level changes were in opposite directions for socially advantaged and non-advantaged people, but neither group experienced statistically significant changes. This finding was robust to excluding varenicline from this variable (Additional file 5: Table 7).
However, the pandemic was associated with changes in behavioral support for smoking cessation and changes in e-cigarette use. Behavioral support utilization increased stepwise by 133.0% (95% CI = 55.3–249.6%), followed by a gradual pre-pandemic decline (Figure 3B). In contrast, e-cigarette use showed a step-level reduction of 21.2% (95% CI = 6.8 to 33.4%) (Figure 3C). This change was short-lived (Additional file 5: Table 3). Because there were also changes in trends that reversed this step-level decline. Before the pandemic, the proportion of smokers using e-cigarettes to try to quit fell by 4.1%. per year; increased by 18.1% per year during the pandemic (RRΔtrend= 1.232, 95% CI = 1.111–1.365, Figure 3C). These changes were similar across sociology grades.
Changes in the use of smoking cessation support were similar even when tobacco dependence was not adjusted for (Additional file 5: Table 4; Additional file 5: Figure 2).







